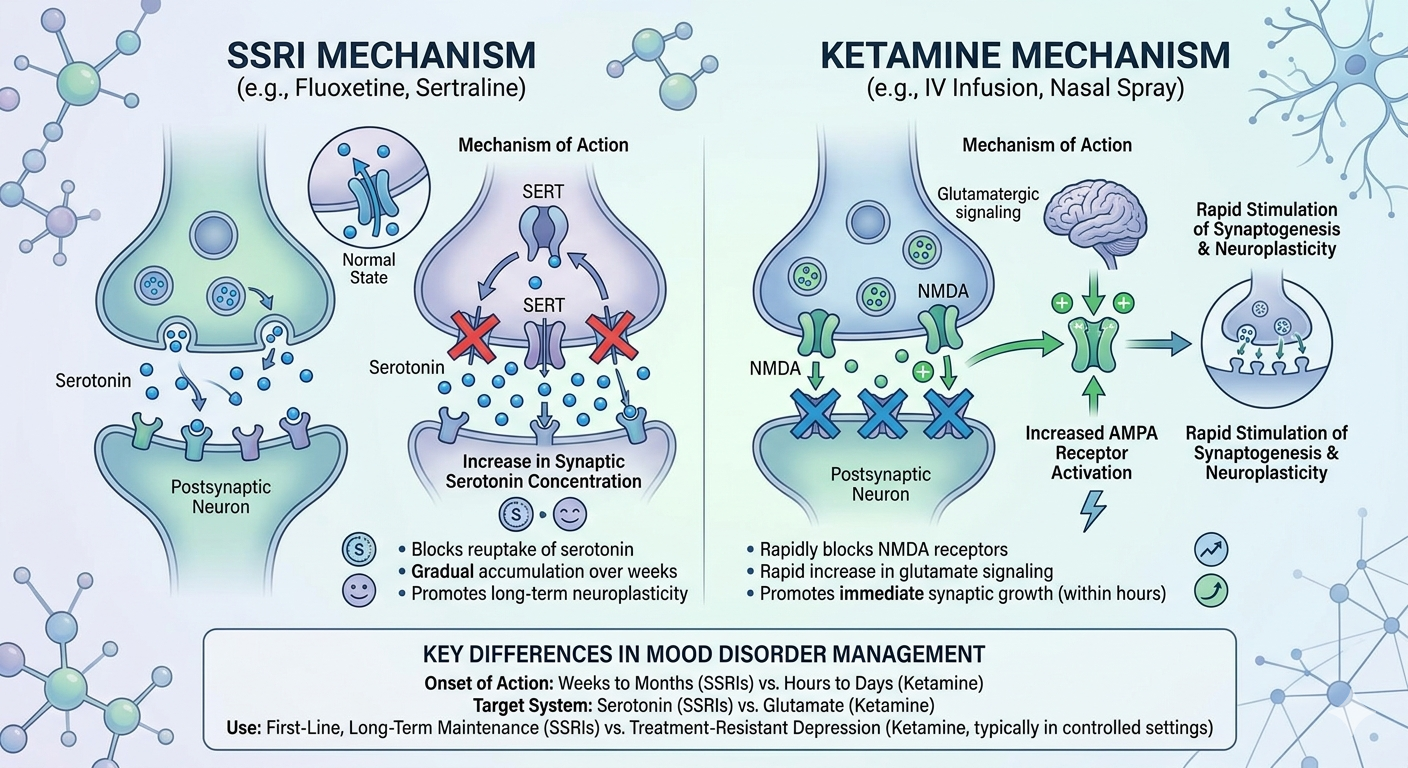
Managing mood disorders such as depression, anxiety, and bipolar disorder often involves a variety of treatment options, each with its own set of benefits and limitations. Ketamine vs SSRI has become a widely debated topic, as both have shown significant promise in managing mood disorders, but they work in fundamentally different ways. SSRIs (Selective Serotonin Reuptake Inhibitors) have long been the go-to solution for treating depression, while Ketamine is gaining attention for its novel approach, particularly for treatment-resistant cases. In this article, we’ll explore how Ketamine compares to SSRIs in managing mood disorders, and why mental health professionals are increasingly considering both as part of a comprehensive treatment plan.
SSRIs: The Traditional Approach to Mood Disorders
SSRIs are commonly prescribed antidepressants that work by increasing the levels of serotonin in the brain, a neurotransmitter linked to mood regulation, happiness, and well-being. Some of the most widely known SSRIs include fluoxetine (Prozac), sertraline (Zoloft), and escitalopram (Lexapro). These medications are often the first line of defense against conditions such as major depressive disorder (MDD), generalized anxiety disorder (GAD), and obsessive-compulsive disorder (OCD).
SSRIs have proven to be effective for many patients, offering significant relief from depressive symptoms. However, the downside is that they can take several weeks to show any noticeable improvement, and not all patients respond positively to SSRIs. This delayed onset can be frustrating for individuals who are struggling with severe mood disorders and are looking for faster relief.
Additionally, some patients experience side effects such as nausea, insomnia, weight gain, and sexual dysfunction while taking SSRIs. For individuals who do not respond to SSRIs or experience intolerable side effects, alternative treatments like Ketamine may offer hope.
Ketamine: A New Frontier in Mood Disorder Treatment
Unlike SSRIs, Ketamine is not a conventional antidepressant. Originally used as an anesthetic, it has gained attention for its off-label use in treating depression, particularly in individuals with treatment-resistant mood disorders. Ketamine works through a different mechanism compared to SSRIs. While SSRIs increase serotonin levels, Ketamine targets the glutamate system, specifically the NMDA receptors. This receptor modulation is believed to stimulate synaptic growth and improve neuroplasticity in the brain, which can provide rapid relief from depressive symptoms.
One of the most remarkable aspects of Ketamine vs SSRI is Ketamine’s rapid onset of action. Many patients experience significant improvements in their mood within hours of administration, whereas SSRIs typically take several weeks to become effective. This immediate relief makes Ketamine an appealing option for individuals who are in acute distress or are at risk of self-harm or suicide.
Ketamine vs SSRI: Key Differences in Treatment
The primary difference between Ketamine and SSRIs lies in their mechanisms of action. While SSRIs work by targeting serotonin receptors and increasing serotonin levels, Ketamine works on glutamate, another neurotransmitter that plays a key role in brain function and mood regulation. This difference in how they function gives each treatment a unique role in managing mood disorders.
1. Speed of Effect
The most notable difference between Ketamine and SSRIs is how quickly they take effect. SSRIs typically take several weeks to show results, which can be discouraging for patients seeking immediate relief from depressive symptoms. For individuals with severe depression or suicidal ideation, the delayed onset of SSRIs can be problematic. On the other hand, Ketamine has been shown to provide rapid relief, with many patients experiencing significant improvements in mood within hours of treatment. This makes Ketamine a potentially life-saving option for patients who need quick intervention.
2. Treatment-Resistant Depression
For patients with treatment-resistant depression, Ketamine is increasingly being considered as a viable alternative. When individuals do not respond to SSRIs or other traditional antidepressants, Ketamine offers a new approach that works differently at the brain’s molecular level. A study published in The American Journal of Psychiatry found that up to 70% of patients with treatment-resistant depression showed improvement after a single Ketamine infusion. This rapid and robust effect makes Ketamine an attractive option for individuals who have exhausted other treatment options.
3. Long-Term Efficacy
While Ketamine is highly effective in the short term, its long-term efficacy is still under investigation. SSRIs, on the other hand, are designed for long-term management of mood disorders. Once a patient responds to an SSRI, they typically continue the medication for months or even years to maintain stability. In contrast, Ketamine may require repeated treatments to sustain its effects, and long-term use can lead to concerns about tolerance, dependency, or potential abuse.
The Side Effect Profile: Ketamine vs SSRI
Both Ketamine and SSRIs come with their own set of potential side effects, though the nature of these effects differs.
- SSRIs: The most common side effects include gastrointestinal issues like nausea, as well as insomnia, sexual dysfunction, and weight gain. These side effects tend to be mild and subside over time, but they can be discouraging for some individuals.
- Ketamine: Ketamine is generally well-tolerated in controlled treatment settings, but it can cause dissociation, hallucinations, and changes in perception, particularly when administered in high doses. Other potential side effects include elevated blood pressure, dizziness, and nausea. These side effects are typically transient and wear off quickly after the treatment session, but they can be more intense than the side effects associated with SSRIs.
Which Treatment Is Right for You?
The decision to use Ketamine or an SSRI for managing mood disorders depends on several factors, including the severity of the disorder, the patient’s response to prior treatments, and the urgency of the situation. For individuals with mild to moderate depression or anxiety, SSRIs may be an appropriate first-line treatment. However, for individuals with treatment-resistant depression, Ketamine offers an alternative that may provide faster and more significant relief.
It’s essential for individuals considering either treatment to work closely with a healthcare provider to evaluate the best course of action based on their individual needs and medical history. A healthcare provider may even recommend a combination of treatments, using SSRIs for long-term management while incorporating Ketamine for rapid relief or to address treatment-resistant symptoms.
Conclusion
In the ongoing debate of Ketamine vs SSRI for mood disorder management, both treatments offer distinct benefits and are valuable tools in psychiatric care. SSRIs continue to be the standard treatment for many individuals with mood disorders, offering effective long-term management. However, for individuals who do not respond to traditional medications or need rapid relief, Ketamine offers a promising alternative with its rapid onset and unique mechanism of action.
As research continues, Ketamine may become a more widely accepted treatment option, especially for those with severe or treatment-resistant depression. Whether Ketamine or an SSRI is the right choice depends on each patient’s individual needs, but with the growing body of evidence supporting Ketamine, it’s clear that it has a significant role to play in the future of mood disorder management.