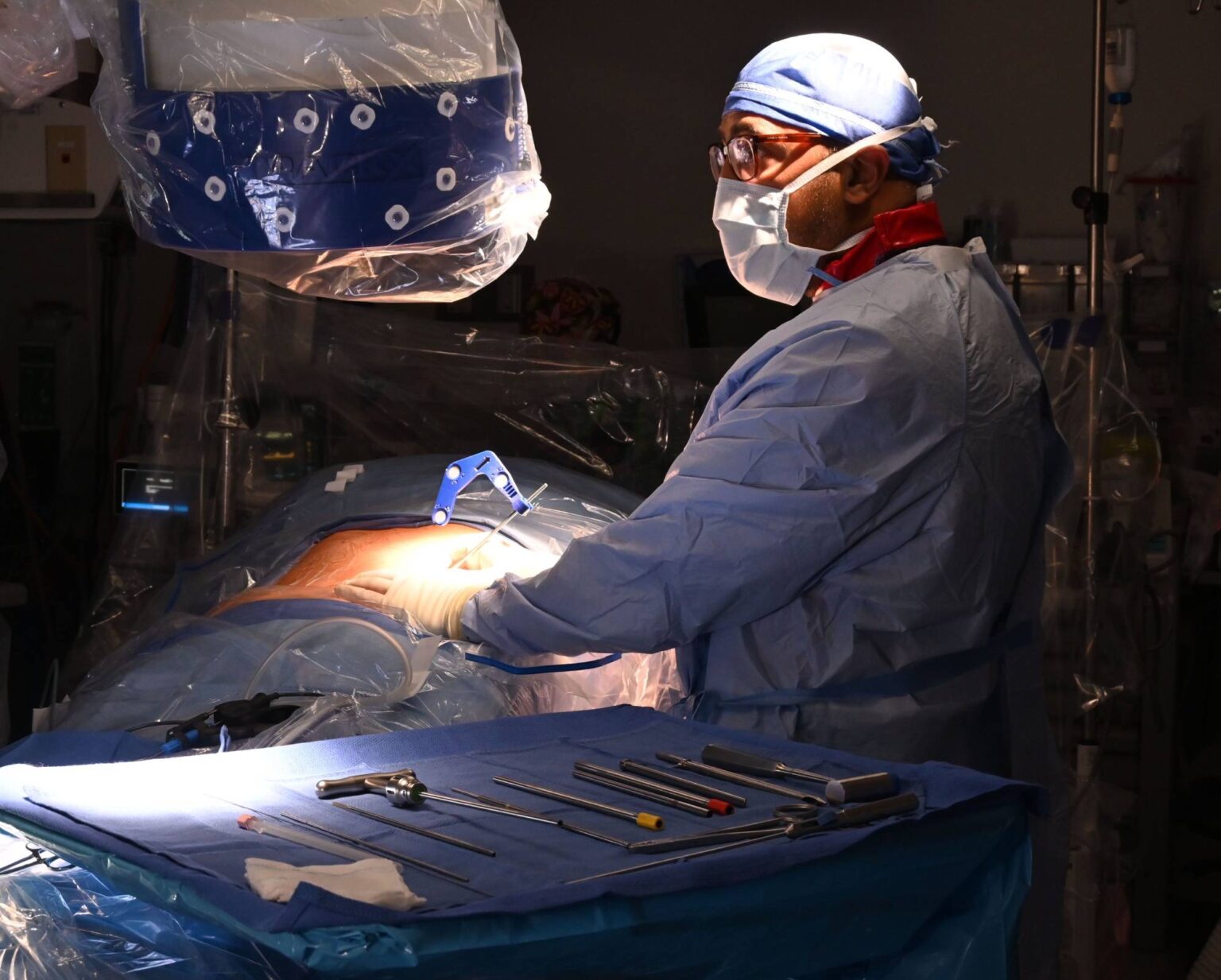
For decades, the mention of “spine surgery” conjured images of long hospital stays, agonizingly slow recovery periods, and the looming fear of permanent nerve damage. For those suffering from chronic back pain, herniated discs, or spinal stenosis, the choice was often a painful stalemate: endure the daily discomfort or undergo a “traditional” surgery that felt as daunting as the condition itself.
Fortunately, medical technology has evolved by leaps and bounds. Enter Endoscopic Minimally Invasive Spine Surgery (MISS)—a revolutionary approach that is redefining what it means to heal. By prioritizing smaller incisions, precision technology, and faster recovery, this technique has transformed surgery from a major life-altering event into a manageable path toward a pain-free life.
What is Endoscopic Minimally Invasive Spine Surgery?
At its core, endoscopic spine surgery is the pinnacle of “keyhole” technology applied to the human spine. Unlike traditional open surgery, which requires a surgeon to make a long incision and strip or retract large sections of muscle to get a clear view of the vertebrae, endoscopic surgery uses a high-definition camera and specialized micro-instruments.
The procedure involves a tiny incision—often less than a centimeter. Through this portal, the surgeon inserts an endoscope, a thin tube equipped with a light source and a high-resolution camera. This allows the surgeon to view the surgical site on a magnified screen in real-time. By navigating through natural tissue corridors rather than cutting through muscle, the surgeon can address the root of the pain—be it a herniated disc, bone spur, or narrowed spinal canal—with pinpoint accuracy.
The Evolution: Open vs. Endoscopic
To understand why this shift matters, it helps to look at the differences between traditional open surgery and the endoscopic approach:
- Muscle Preservation
In open surgery, the muscles surrounding the spine are pulled away from the bone to create a “window.” This retraction can lead to muscle trauma, post-operative pain, and sometimes long-term weakness. In endoscopic surgery, the instruments gently push the muscle fibers aside without cutting them. The muscles remain intact, leading to significantly less post-surgical pain.
- The Incision Size
Open surgery often necessitates a multi-inch incision. Endoscopic surgery, by contrast, usually requires an incision no larger than a dime. This not only minimizes scarring but also drastically reduces the risk of post-operative infection.
- Precision and Magnification
While the human eye is precise, it has its limits. An endoscope provides a magnified, clear view of deep anatomical structures, allowing surgeons to distinguish between nerve tissue and the structural issues causing pain with incredible clarity. This precision minimizes the risk of incidental nerve damage.
Who is a Candidate?
While not every spinal condition requires surgery, and not every spinal surgery is suitable for an endoscopic approach, this method has become the gold standard for many common issues, including:
Lumbar Herniated Discs: The most common application. Surgeons can remove the fragment of the disc pressing on the nerve, providing immediate relief from sciatica.
Spinal Stenosis: For those suffering from the narrow spaces in the spine, endoscopic techniques can remove the bone or ligament overgrowths that are compressing the spinal cord.
Foraminal Stenosis: When the nerve exit points in the spine become clogged, endoscopic surgery can clear the pathway with minimal bone removal.
Patients who have failed physical therapy, chiropractic treatment, or epidural injections—and who are looking for a long-term solution without the burden of a traditional hospital recovery—are often the ideal candidates.
The Recovery Journey: Getting Back to Life
The most striking advantage of endoscopic spine surgery is the recovery timeline. Traditional back surgery often mandates a significant hospital stay and weeks, if not months, of downtime.
Because endoscopic procedures are minimally invasive, most are performed on an outpatient basis. In many cases, patients walk out of the surgery center just a few hours after the procedure is completed.
What can you expect in those first few days?
Reduced Pain: Because the muscles were not cut, the “aching” sensation usually associated with back surgery is significantly dampened.
Early Mobilization: Doctors encourage patients to walk almost immediately. Movement is encouraged to prevent stiffness and promote natural healing.
Return to Work: Depending on the physical demands of your career, some patients return to light duty within a few days to a week.
While it is still “surgery,” the emotional and physical toll is significantly lighter. The fear of being “out of commission” for months often fades when patients realize they aren’t starting from scratch after the procedure.
Debunking the Myths
Despite its success, some patients remain hesitant. Let’s clear up some common misconceptions:
Myth #1: “It’s not as effective as open surgery.” Studies have consistently shown that for specific conditions like disc herniation, endoscopic techniques yield outcomes that are equal to, or better than, open procedures, with significantly lower rates of post-operative complications.
Myth #2: “It’s ‘experimental’.” Endoscopic spine surgery has been refined over several decades. It is a mature, evidence-based surgical specialty that is practiced by highly trained surgeons worldwide.
Myth #3: “If it’s ‘minimally invasive,’ it’s not a ‘real’ surgery.” Make no mistake: it is a surgical procedure. It involves anesthesia, precise navigation of anatomy, and technical skill. The “minimally invasive” label refers to the approach to the spine, not the severity of the procedure itself.
Choosing the Right Path
If you are living with back pain, the first step is always a thorough diagnosis. Chronic pain is not merely a nuisance; it is an indicator that something is not right within the body’s structural framework. When non-surgical options are exhausted, endoscopic spine surgery offers a bridge back to quality of life.
However, success depends on the surgeon. Endoscopic surgery has a steep learning curve; it requires a steady hand and extensive training with specialized optics. When looking for a provider, ask about their volume of endoscopic procedures—not just how many total surgeries they perform, but how many endoscopic surgeries they conduct annually.
A Future Without Limits
We live in an era where we no longer have to accept chronic pain as a permanent state of existence. The transition from massive incisions to microscopic portals is more than just a technological upgrade—it is a human one. It respects the integrity of your body, minimizes your downtime, and gets you back to what truly matters: playing with your kids, hitting the golf course, or simply living your daily life without the shadow of pain following your every move.
If you are suffering, don’t let the fear of “traditional” surgery keep you in agony. The future of spinal care is here—it’s smaller, faster, and remarkably effective.